Treatment of Ovulatory Disorders
Published: 12/10/2015
Ovulation is the release of an egg from a follicle in the ovary. Eggs start developing in the genital ridge of an early embryo as germ cells. At the most, there are about 1300 germ cells, that over the ensuing weeks prolifically divide and begin to migrate to the future ovary as eggs. A 20 week old embryo has about 7-8 million eggs; at birth, that number is down to about 1 million; and by a young women's first menstrual cycle, at around 12.3 years old in the US, she is down to about 400,000 eggs. Then, every month a woman ovulates one egg, she losses a 1000.
Each month, one random egg follicle is "selected from those thousands", and becomes known as the "dominant" follicle; the one egg that is destined to be released. Once an egg is released from the ovary, it is thought to live for only 12-24 hours. Typically, a woman will release one egg per month but some women have the genetic propensity to release two or more, resulting in natural twinning (1 in 90) or natural triplets ( 1 in 8100) or natural quads (rare at 1 in 729,000). This continues for the next forty years, every month, until she runs out of eggs, known as menopause, typically at 51.3 years old in the US.
Follicle or egg development (which are commonly interchanged) develops under the influence of FSH (follicle stimulating hormone), which is secreted from the pituitary gland. As the egg follicle grows it produces estrogen (E2). As estrogen increases and peaks, it triggers the release of LH (leutinizing hormone) that triggers ovulation. HCG, used as the trigger shot for timing of IUI is almost identical to LH. Once ovulation occurs and the egg is released from the follicle, the follicle is transformed into a corpus luteum (CL), which begins production of progesterone (P4) to help prepare the lining of the uterus in anticipation of a possible pregnancy, and support that early pregnancy until the placental hormones fully take over at 12 weeks.
Loss of the corpus luteum (CL) before 8-10 weeks, for whatever reason, i.e. surgery, will result in a miscarriage unless the woman is given supplemental natural progesterone. If pregnancy does not occur, than this process abates around day 23 of the cycle and the lining of the uterus starts to shed (menstruation) around day 28 and the whole cycle begins again. Not such a great design, is it?
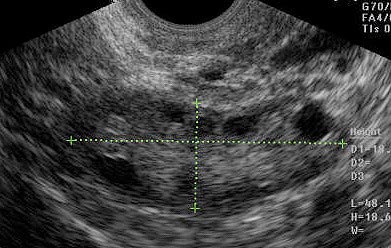
Understanding the endocrinology of the menstrual cycle is critical because it is the foundation for maximizing successful results with fertility treatments, particularly IUI and IVF
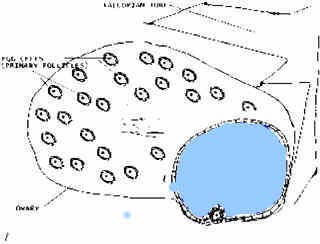
Picture 1 - Pre-Ovulatory Dominant Follicle
Basal Antral Follicle (BAF) Count
Graphic representation (Picture 1) of a pre-ovulatory dominant follicle around the time of ovulation. An early ultrasound (Picture 2) at the start of a cycle (typically day 1-2) can show all pre-follicles, or what is known as BAF, basal antral follicle count. From these pre-follicles, the dominant follicle is randomly selected. BAF's are important in predicting the number of dominant follicles (eggs) a woman will make for egg recovery for IVF, if adequately stimulated for her age and reproductive genetics. The below ultrasound shows an ovary with a BAF of 8 (make sure to count the tiny antral follicles).
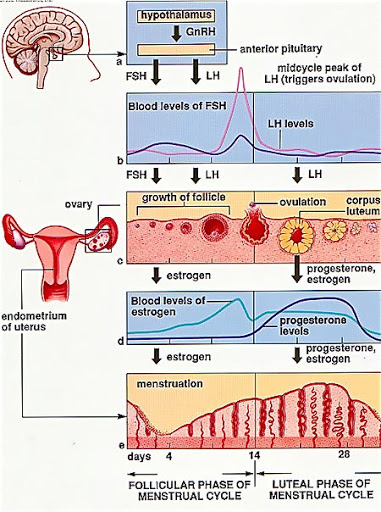
Picture 2 - Ultrasound showing BAF (Basal Antral Follicle Count)
Corpus Luteum (CL)
Early corpus luteum (CL) just after ovulation has occurred (picture 3). The follicle undergoes some complex steps, after the egg is released, to transform into a corpus luteum, to produce progesterone, to prepare the lining of the uterus for an "anticipated" pregnancy; and if implantation occurs, early hormonal support of the pregnancy, until the placenta takes over.
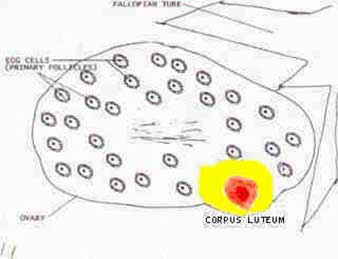
Picture 3 - Corpus Luteum
Ovulatory Disorders
Ovulation generally occurs on a regular monthly basis. Anything that interferes with this process can cause ovulatory dysfunction and ovulatory disorders. Generally, if a cycle is less than 21 days or longer than 38 days, the woman is not ovulating or is anovulatory. Woman with premenstrual symptoms and regular periods are ovulatory 97% of the time. 3% of the time, a woman with regular cycles is not ovulating. If a woman's cycles are irregular, say between 1-6 months apart, she may occasionally ovulate, which is called oligo-ovulation.
Circumstances that can cause ovulatory disorders are:
- Physical, emotional and psychological stresses
- Polycystic ovarian disease (PCOD)
- Disorders of the pituitary, adrenal or thyroid glands
- Elevated prolactin levels
- Excessive exercise
- Breast feeding
- Very low body weight
- Obesity - 25% over ideal body weight
- Idiopathic - unknown or no obvious reasons
Predicting Ovulation
Ovulation can be predicted by several different methods, which can be helpful in timing intercourse or insemination.
Basal Body Temperature Charts (BBT)
Basal body temperature charts are generated by taking your daily resting morning temperature (prior to getting out of bed, kissing your partner and at the same time each day) for 3-6 months and graphing the temperatures on a chart.
In the first half of the cycle, or follicular phase, temperatures are low around 97-98 degrees; but with ovulation and the production of progesterone (luteal phase of the cycle), which is thermogenic and causes a 0.4-1.0 degree raise in the resting basal temperature, the temperature begins to go up and peaks out approximately 36 hours after ovulation and continues to stay elevated unless you are not pregnant and falls back to follicular levels with the onset of the menses.
BBTs are useful in showing a pattern of ovulation, but only in retrospect. Since an egg only lives for 12-24 hours, by the time the temperature is elevated the egg is no longer viable. Also, BBTs are a pain in the neck to do every morning, let alone read the thermometer when you are half asleep.
Arizona Center for Fertility Studies does not recommend doing BBTs and has never met a patient who got pregnant by "taking her temperature". Understanding how and when ovulation occurs and the fact that sperm live in the reproductive tract for 3-4 days (in the cervix) is a much easier and more "fun" way of getting pregnant.
Ovulation Detection Kits (ODK)
Ovulation detection kits, which can be purchased over the counter, measure the LH surge in the urine and once positive, predict ovulation within 26-40 hours. They are more accurate and less troublesome than BBTs, and if you want to play "junior chemist" are a good way of determining when to have intercourse. Although, Arizona Center for Fertility Studies is not opposed to recommending ODK to predict ovulation, again, a simple understanding of the menstrual cycle is a lot less expensive.

One of the more popular over the counter ovulation detection kits or ODK
Inducing Ovulation With Fertility Medications
Once it is determined that you are not ovulating on a regular basis, and all other medical conditions have been ruled out and/or treated (thyroid disease or elevated prolactin, etc.), "fertility" medication will be recommended to induce regular ovulation.
If you have not had a menstrual bleed in over 40+ days, a urine pregnancy test is done and if negative, given either oral progesterone (Provera) for 5 days or a shot of natural progesterone in oil (100 mg IM) to induce a bleed. Bleeding should occur within 3-7 days but up to 14 days. Once bleeding occurs, that is cycle day 1, and you are to call the office to schedule an ultrasound to rule out any ovarian cysts.
Choices for medication to induce ovulation include:
Clomid
Clomid, which is an anti-estrogen, competes with estrogen receptors on the hypothalamus and tricks the body into thinking there is no estrogen around. First introduced as a birth control agent, which failed miserably, it was quickly appreciated to be able to treat ovulatory disorders by causing the increased production of FSH by the pituitary, and begin the ovulation process. As long as the estrogen level was not too low (you had a bleed from progesterone; no bleed indicates that estrogen is already too low and Clomid cannot trick the body into thinking it is any lower), Clomid induces ovulation around 85% of the time, with a pregnancy rate of about 45% and multiple rate of 8%.
Clomid should work within 3-6 cycles, and if not, it should be discontinued. The dose is started off at 50 mg daily, days 3-7 or 5-9 of the cycle, and can be increased in increments of 50 mg, only if ovulation does not occur. Side-effects of clomid include-ovarian enlargement, hot flashes, abdominal discomfort, breast tenderness, nausea, vomiting, visual symptoms, headache, abnormal bleeding, and multiple births. Many woman do not have these side-effects and for the majority that do, they tend to be mild. A few women will never take the medication again after being on it for one cycle. If, however, any visual symptoms or severe headaches occur, Clomid has to be discontinued immediately and never used again.
Because of the anti-estrogen properties of clomid, not only are the estrogen receptors in the hypothalamus blocked, but those on the cervix and uterine lining as well. This can result in blocking estrogen receptors on that part of the cervix that produces cervical mucus and thus interfering with the sperm-mucus interaction and preventing pregnancy. Interfering with the estrogen receptors on the lining of the uterus may interfere with the lining being properly prepared for implantation and result in not getting pregnant and/or increasing the risk of a miscarriage. If clomid is to be used, Arizona Center for Fertility Studies recommends that on the first cycle of use, a PCT) is done to check the sperm-mucus interaction, as well as an EMB to rule out a luteal phase defect. If the PCT is abnormal, IUI can be done and if the EMB is out of phase, progesterone can be started and the biopsy re-checked.
Clomid should not be used in normally ovulating woman; unfortunately a common practice among many doctors, because, in these circumstances, it has been shown not to improve fertility rates. Far too often, Clomid is routinely given to women who "are having trouble getting pregnant", and if they do not get pregnant on that cycle, the dosage is increased, in 50 mg increments, on each consecutive cycle they are not successful; only increasing the costs, side-effects and not changing the chances of conception. Because of its anti-estrogen effects on the cervix and lining of the uterus (endometrium), rather than Clomid enhancing a woman's fertility, it can actually decrease it.
Arizona Center for Fertility Studies, does not recommend Clomid being given to women with regular cycles unless it is being used along with IUI and a previous EMB showed no interference with the endometrial lining.
FDA guidelines state that Clomid should only be used for 6 cycles in a lifetime because of the increased risks of ovarian tumors.
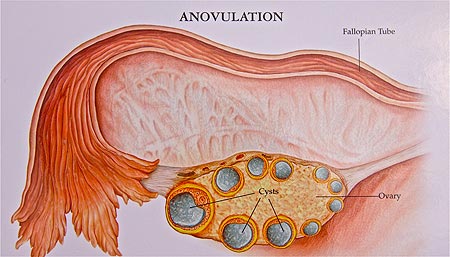
Graphic representation of anovulation or failure to make and release an egg where the ovary contains multiple small cysts on ultrasound
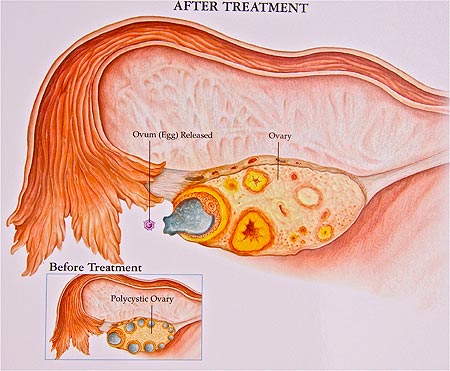
Graphic representation of the ovary showing ovulation or release of the egg after Clomid administration. The same would be true if gonadotropins were used. Clomid causes the release of 1-3 eggs; whereas, gonadotropins cause the release of 2-5 eggs, both depending on the age of the woman.
Gonadotrophins
Gonadotrophins are medical preparations of naturally occurring hormones that are basically identical to the signals sent by the pituitary to stimulate follicular development of the egg. They include:
| Repronex | or HMG (human menopausal gonadotrophin) equal amounts of 75 IU of FSH and 75 IU of LH, manufactured by Ferring, Inc. |
| Follistim | 75 IU of FSH, manufactured by Organon, Inc. |
| Gonal-F | 75 IU of FSH, manufactures by Serono, Inc. |
In cases of ovulatory dysfunction where clomid has not been successful or the woman chooses to be more aggressive in her treatment, gonadotrophins are used to bypass the body's normal process of egg production, development and release. Ovulation rates approach 100%, pregnancy rates are approximately 75%, with the risks of multiples being around 15-20% only in younger patients, which if monitored properly should be only twins. There is no limit in the number of cycles gonadotrophins can be used and there is no FDA warning.
Side-effects of gonadotrophins use include abdominal tenderness, bloating, fluid retention and weight gain. In Arizona Center for Fertility Studies experience, as a natural product, they produce considerably less "emotional and annoying" side effects than Clomid and are better tolerated.
One serious side-effect of gonadotrophin use, and much less so Clomid use, is the risk of ovarian hyper stimulation syndrome or OHSS. The pathogenesis of ovarian hyperstimulation syndrome is unknown, but the process is related to increased vascular permeability in the region surrounding the ovaries and their vasculature. This causes increasing amounts of fluid and protein from the vascular (blood vessels) system to spill into the abdomen. The protein can be irritating to the bowels causing nausea and diarrhea. The increasing accumulation of fluid in the abdomen causes abdominal distention and discomfort, along with increasing weight gain. In its severe form, the fluid accumulation is so significant that it can push up on the diaphragms and cause shortness of breath and labored rapid breathing. Because of the loss of fluid from the vascular system, there is decreased urine output from the kidneys to try to compensate for the loss. In severe stages of OHSS, there is a risk that the kidneys can shut down and subsequently sustain damage.
General reported rates of OHSS are as follows:
| Mild | 8-23% |
| Moderate | 1-7% |
| Severe | 0.25-1% |
Although there is no "cure" for OHSS, management for the mild and moderate forms is straight forward and involves fluid and electrolyte replacement trying to alleviate the accompanying symptoms of nausea and diarrhea. The severe form occurs less than 1% of the time and requires hospitalization and strict fluid and electrolyte management and will eventually resolve itself. Severe OHSS only seems to occur if the woman gets pregnant; therefore, if a patient is at an increased risk of developing OHSS, hCG is not given. In the case of IVF, it is okay to give hCG to trigger ovulation and recover and fertilize the eggs but no transfer is done. The embryos are frozen and then later transferred in a non-stimulated cycle. In the last 10 years, Arizona Center for Fertility Studies has not had a single case of severe OHSS.
If the patient is at increased risk of developing moderate and/or severe OHSS, Arizona Center for Fertility Studies will trigger the release of the eggs with Lupron instead of with hCG. By triggering with Lupron you will be able to completely avoid the risks of developing ovarian hyperstimulation syndrome (OHSS). The downside of triggering with Lupron is that you will not be able to do a transfer because you do not make corpus luteum (which make progesterone that supports the uterine lining and will have to freeze all the embryos; and subsequently do a frozen embryo transfer transfer.
The decision to trigger with hCG versus Lupron is based on a number of criteria:
- Estrogen levels greater than 5000 pg/ml at the time of trigger.
- There is data to suggest that when the reproductive system is "over-stimultated" that it may not be the "best" environment for pregnancy to occur and it is subsequently better to transfer in a prepared cycle. You should not, however, hold back on "appropriate" stimulation for a given patient just to do a fresh transfer. If you are not given the "appropriate" amount of hormonal stimulation for your age and based on experience; you may avoid OHSS and Lupron trigger, but might "under-stimulate" and end up with either a decreased amount of eggs/ embryos or poor egg/embryo quality or both.
- Whether or not the patient is already developing symptoms of OHSS like abdominal pain, bloating, weight gain, breast tenderness, nausea and just generally feeling "lousy".
- If the patient is already doing PGD/PGS: 23-chromosome microarray with a day 5/6 TE biopsy and doing cryopreservation anyway.
- By triggering with Lupron instead of hCG, you can stimulate the more aggressively; thus get more eggs/embryos and not worry about the risks of OHSS; which is a distinct advantage when there is an benefit of having more eggs/embryos.
Repronex, made by Ferring, is 75 IU of FSH and 75 IU of LH, and is administered intramuscular (IM)
Follistim, manufactured by Organon, contains only 75 IU of FSH is can be given sub-cutaneously (sub-Q) or intramuscular (IM)
Unlike Clomid, gonadotrophins (HMG and FSH) are daily intramuscular (IM) orsub-cutaneously (sub-Q) injections and have to be monitored carefully and more judiciously than Clomid, as well as for the risk of OHSS. A woman calls on the first day of her cycle to have an ultrasound to rule out any ovarian cysts. For IUI, low dose gonadotrophins are begun on cycle day 5, and when stimulating for IVF, high doses are started on cycle day 3. Ultrasounds are done every 2-3 days to monitor and follow follicular (egg) growth, and when the follicles are mature and18 mm in size, 10,000 IU of hCG is given to trigger ovulation. With gonadotrophin use, unlike Clomid, ovulation does not occur spontaneously and has to be triggered with hCG. In the case of IUI, insemination is done around 42-43 hours; and with IVF, the eggs are recovered at 36 hours, one to two hours before the process of ovulation starts.
The idea is that since every month 1000 eggs are lost for each one that eventually ovulates, increased stimulation with gonadotrophins for IVF will recover some of those eggs that are normally going to be lost. In your 20's, you can recover about 1.5% or 15 eggs; in your 30's about 1% or 10 eggs;and in your 40's about 0.5% or 5 eggs. These are just estimates and any age group can develop more or less.
With IUI the goal is only to make 2-4 eggs for insemination in order to decrease the risk of multiples and only low-dosage gonadotrophins are used. With IVF, the goal is to use high-dosage gonadotrophins, balanced with avoiding OHSS, in order to have more embryos to choose from, so as to be able to put back the "best" and freeze extras for future pregnancies and not have to go through another stimulation cycle.
Human Growth Hormone
ACFS has successfully used hGH (human growth hormone) for many years; mainly in IVF stimulation protocols. FSH and LH are the two main gonadotropins that are the signals from the brain to the ovary. They not only initiate egg and follicular development, but are necessary for the full and final maturation of that egg and follicle and preparation of the uterine lining for implantation. HGH is a co-gonadotropin, also needed for the full and final maturation of an egg/follicle. The pituitary gland releases all three hormones at precise timing each cycle causing ovulation (release of the egg from the follicle) and preparation of the uterine lining for a pregnancy to implant. If pregnancy does not occur, the withdrawal of FSH and LH stimulation results in menstrual bleeding (sloughing off the lining of the uterus or endometrium) and resetting the hypothalamus/pituitary for next months' (cycle) stimulation. HGH is needed in this process and is essential for the full and final maturation of the cycle's egg and follicle. Without it, there will not be full and final maturation of the egg and follicle. Normally, the pituitary secretes enoughhGH for this maturation. The question is, because of the high dose IVF stimulation protocols, designed to stimulate and recover "alot" of mature eggs, (hyperlink to this section: The idea is that since every month 1000 eggs are lost for each one that eventually ovulates, increased stimulation with gonadotrophins for IVF will recover some of those eggs that are normally going to be lost. In your 20's, you can recover about 1.5% or 15 eggs; in your 30's about 1% or 10 eggs;and in your 40's about 0.5% or 5 eggs. These are just estimates and any age group can develop more or less. The questions becomes, "is there enough hGH to go around" to effectively stimulate the needed maturation of all these extra eggs and follicles"? Women were never supposed to make more than one egg per cycle, so years ago when IVF stimulation protocols allowed for multiple eggs to develop, ACFS wondered and asked the question, "Does the body (hypothalamus/pituitary gland), in any age group, secrete enough hGH for the full and final maturation of all the extra eggs that are being produced as result of more aggressive IVF stimulation protocols"? As a result, ACFS measured hGH levels in all patients, regardless of their age, undergoing IVF to see if certain patients " could be identified" that had low levels and could benefit from supplemental hGH injections. Not to our surprise, all patients had normal growth hormone levels. But the one question that was not answered was, although patients' hGH levels were normal, did they have enough hGH needed for the full and final maturation of all the extra eggs that were being produced; as measured by egg maturity, fertilization rates, normal blastocyst development and currently, chromosomally normal (euploid) embryos. It made sense that there would be patients, especially those that "make alot of eggs" or are "reproductively older" that could benefit from the addition of hGH supplementation. A number of years ago, our early experience of supplementing IVF stimulation protocols with hGH showed improvement in egg maturity and subsequent embryo quality. Although, not all patients need or will benefit from hGH supplementation (unfortunately, they can not be identified), ACFS believes that it can make a difference in IVF outcomes by increasing the possibility of better egg and embryo quality which would subsequently help to improve pregnancy rates and reduce miscarriage rates. Now, with years of experience using hGH supplementation with IVF stimulation protocols, ACFS continues to recommend its use. We have had not seen a single side effect and/or adverse reaction with its use and subsequently have incorporated hGH in our IVF stimulation protocols.











