Blastocyst Transfer
Published: 12/11/2015
The principal cause for In Vitro Fertilization (IVF) not being successful is the failure of the embryo(s) to implant in the uterus after transfer. It is unclear why this should be, but various modifications of the In Vitro Fertilization (IVF) treatment have been tried to improve the chances of implantation. One of these is Blastocyst Culture.
Most embryo transfers are done on day 3 after egg collection. Some embryos do well in culture while others do not. It is hard to tell which type of embryos you have. If embryos are cultured in the laboratory for a longer period of time (days 5-6), they may develop further to the Blastocyst Stage. At this stage, the embryo has differentiated and is made up of more than 100 cells and it is possible to identify groups of cells that will make up the placenta (trophectoderm cells) and the fetus (stem cells).
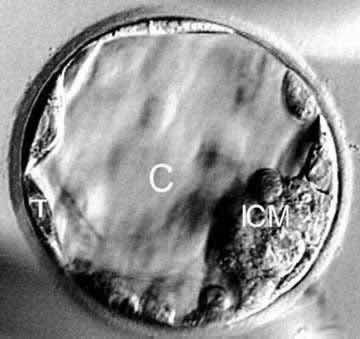
A nice looking day 5 blastocyst with an ICM, inner cell mass or stem cells, a blastocyst cavity (C), and a ring of outer cells, known as trophectoderm, that will develop into the future placenta.
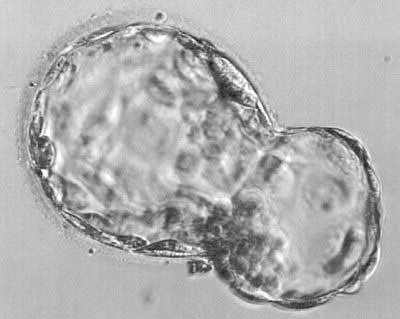
Picture of a very nice looking day 6 "hatching" blastocyst. This is where the blastocyst begins to break out of its shell (zona pellucida), getting ready for implantation on cycle day 6-1/2 from fertilization.
Criteria To Consider Before Blastocyst Transfer
Growing embryos in the laboratory is a difficult process and the longer that they remain in culture the greater is the chance that some or all of the embryos produced by the In Vitro Fertilization (IVF) process will not survive. On the other hand, in an excellent IVF laboratory with an experienced and skilled embryologist, many embryos will survive to day 5-6 or the blastocyst stage and are believed to have a greater chance of implanting. Using new and advanced blastocyst culture methods, the ability to grow embryos to the blastocyst stage has significantly improved. Said differently, only the "best of the best" embryos make it to the blastocyst stage. Since blastocysts are "very good embryos" they tend to freeze and thaw very well.
On the other hand, good day 3 embryos also freeze and thaw well. However, for the last 5-6+ years, ACFS has cultured all their patients’ embryos to the blastocyst stage with excellent results. ACFS can say we confidence, that if your embryos do not make it to day 5-6 in ACFS in-vitro culture environment, they would not have been successful even if transferred on day 3. Since only the “best of the best” make it to the blastocyst stage, that is very important information to have, because by not waiting to see if day 3 embryos can make it to the blastocyst stage, you may be doing a lot of transfers that will not be successful. Obviously, someday 3 embryo transfers can be successful but in ACFS's opinion, those would have been the embryos that would have progressed to day 5-6 anyway; unfortunately, you can not identify them in advance.
Some clinics feel that the uterus is a “better” environment than the IVF laboratory. ACFS respectfully disagrees and strongly feels that in our culture system; all good embryos, regardless of the patients’ age, can develop successfully to the blastocyst stage. And if they do not, they would not have been successful if transferred on day 3.
Based on our long and extensive experience with embryo culture, Arizona Center for Fertility Studies strongly recommends growing all embryos to the blastocyst stage (day 5). In our experience, ACFS gets much higher pregnancy rates with a day 5 blastocyst transfer. A couple should understand that there are a few animal studies that have raised concerns about neonatal problems such as increased birth weight and fetal abnormalities. There is no evidence at the present time of similar problems following the transfer of human blastocysts.











